

Design Thinking in Digital Health for Patients and Clinicians
Healthcare has seen tremendous stride in delivery methods with the advent of new technologies in telemedicine, remote patient monitoring, and patient engagement & communication. However, technology has outpaced the rate at which healthcare can keep up with technology and effectively implement it within clinical workflows and operational setting. This coupled with the slow pace of
progress within healthcare leaves patients, clinicians, and administrators with mismatched capabilities and needs. A good example of this is telemedicine, many states do not have parity laws, reimbursement is not standardized across the nation, and physicians must be licensed to provide services across state lines (physicians at the VA are not subject to the latter). For providing healthcare within rural America, telehealth faces further complications due to unavailability of resources and access to (remote) care. Typically, technological growth and innovation outpaces an industry’s ability to keep up.
Another issue that healthcare faces is the rapid expansion of technology beyond the users ability to keep up. Technology not only outpaces industry & organization but users as well; for how often are there digital solutions implemented within healthcare leaving users with little means of using it. Clinicians far too often are challenged when using EMR and related clinical systems for managing patient care. A University of Wisconsin School of Medicine and Public Health and American Medical Association study?with 142 family-medicine physicians found that physicians spend around 52% of their 11.4 hour workday on the EMR. The high cognitive demands and workload leave physicians with less time to focus on their patients and managing patient care. Whether digital health technology is outpacing healthcare organizations or outpacing clinicians & patients, there is a clear need to better integrate people, organizations, and technology.
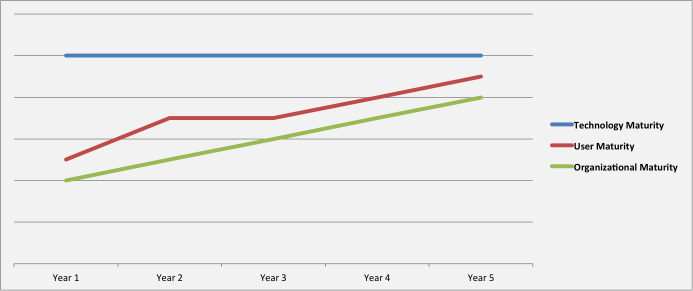
Figure 1. Socio-technic maturity. Source: Derived from concepts in Orchestrating Human-Centered Design.
This a complex problem that has to be approached by all stakeholders within healthcare – organizations, clinicians & administrators, and digital health innovators. Organizations need to better understand technology and user needs as well as develop effective strategies to implement technology. Digital health innovators need to better understand the needs of organizations and users. Users need to be approached by organization and digital health companies to better understand what users really need and want.
What is required in this case is a holistic approach where Technology, People, and Organizations are equal stakeholders and influencers. Within the field of human-centered design and design thinking, a drastically different approach is taken where users are at the forefront of product/process design. We begin by understanding user needs, usability, and what is the problem we are trying to solve. Next is to understand how can we solve the problem, followed by testing the solution and gaining feedback from users until it is ready for use.
While many telehealth companies do focus on understanding user needs, we must not forget how the organization will operate the technology.
Technology
Developers of telehealth and other digital health tools must begin from what problem they are trying to solve.
- What is the purpose of the product?
- Who will use the product?
- How will users use the product?
- Will the product take more effort than expected by the users?
Answering these questions will often lead to more questions, the crux being that Developers aren’t so much as creating a product as they are solving a problem users have. Addressing the above questions requires use of human-centered design methodologies such as design thinking and usability assessment.
People
Developers and application users need to be on the same page. To identify what problems Users face and what are the barriers to care, we must identify what are the pain points of Users (who assumedly are Clinicians, Patients, and or Administrators). Begin by understanding what the users really want as opposed to what we think they want; as Suzzane Gibbs Howard at IDEO U points out, by using design thinking principles, we can gain deeper understanding of user needs and wants. Empathizing with users can result in stronger collaboration and better feedback. Thus yielding clarity regarding what users really feel and want.
Deeper brainstorming and planning using specific human-centered design techniques such as User Journey Maps, Scenario-based Design, and User Personas can help translate User needs and pain points into specifications.
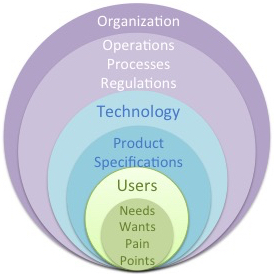
Figure 2. Human-centered design approach to product development.
Organization
When any system is implemented at a (large) organization, unexpected complexities arise leading to delays, cost escalations, and frustration. Furthermore, end-users are not always consulted to determine their needs and wants. A good example in healthcare is large-scale implementation of EHR systems that create financial burden on hospitals, increase workload, and reduce Clinician efficiency leading to fatigue. As Dr. Arlen Meyers points out, ‘technofatigue’, the fatigue experienced by dealing with complications arising from use of technology can considerably increase Clinician fatigue. Both hospitals and EHR companies are guilty of building and deploying systems without considering the impact on the end-users. Fatigue, workload, operational burdens are an afterthought. In fact, hospitals can harmonize operational needs, technology selection, and user needs using human-centered design. Hospitals can determine user needs using design thinking walkthroughs, test products using technically validated usability tests such as the System Usability Scale (SUS), NASA Task Load Index (TLX), and more complex assessments such as Heuristic Evaluations.

Figure 3. Feedback process in human-centered design product design.
Additionally, hospitals should focus on collaborating with health technology companies to determine system needs, specifications, and feature-set. However, rather than focusing on purely technical requirements, consideration should be given at early stage to building product design using scenario-based design (user and organizational input in how they would use the system) and low & high-fidelity prototypes for testing the system.
Human-Centered Process
The process of understanding and solving a problem using design thinking and human-centered design has five primary steps:

Figure 4. Steps to design thinking
Empathize
Whether you are building your product for Clinicians, Patients, or Administrators, focus on seeing things from their perspective. Ask them to provide deep insights regarding their pain points, frustrations they face when dealing with a technology, and barriers that inhibit their progress. Understand the users desire and motivation to undertake specific actions. Leave aside any biases you may have and focus on the user.
Define
Upon understanding user needs and shortcomings to address those needs, develop a holistic and organic problem statement that addresses user needs and organizational goal. The crux here being that you are formalizing and structuring the concepts and knowledge elicited during the previous phase.Defining the problem can begin with a problem statement with additional specific points of concern.
Ideate
Develop concepts for addressing the problem(s) you have identified, have a multi-disciplinary team generate wide-array of ideas for tackling the problem. The first part of ideation should focus on breadth of ideas and concepts – think beyond conventional concepts. There are myriad of ideation techniques for concept generation, knowledge stratification, and specification development. Some ideation techniques are brainwriting and group-elicitation method (GEM). Once you progress through the breadth of concepts, begin narrowing down to building on specific concepts and themes; build on the concepts till you can derive functionalities and feature-set. A helpful technique to use at this phase is scenario-based design.
Scenario-based design has the following elements:
- User persona – describe the typical user taking into account social, technological, mental, physical, and cultural factors.
- Task – describe actions the user would undertake to fulfill the task
- Narrative – build a narrative of user actions to complete a task during a normal day-to-day operation. Keep the narrative simple as if it were a story
Prototype
Based on the concepts and features generated during the ideation phase, build a prototype of the product. The prototype could be low-fidelity such as paper-based prototype to simulate digital health tools, they can be high-fidelity software-based prototypes, or they can be mixed-fidelity (mixture of high and low-fidelity). The main point is to build a prototype that is built from user input and concept refinement.
Test
Upon prototype completion, test the prototype with users. If possible, include expert users, usability experts, and the typical end-user. Based on the feedback received from the users, refine the prototype until it is ready for deployment. During testing, multiple usability testing can be conducted to determine how well designed is the prototype. Usability tests such as system usability scale, heuristic evaluation, and cognitive walkthroughs can be used to conduct formalized and technically valid tests.
Human-Centered Design at DocToDoor
At DocToDoor, we utilize human-centered design principles in multiple ways. As a multi-disciplinary including human-centered design expert, we focus on reducing user workload & cognitive demand, improving Clinician capability & situational awareness, and improving Patient engagement & outcomes.
Our focus is on reducing the time and effort required by clinicians to manage patients and analyze data. By improving usability, increasing automation, and presenting critical patient-generated data in meaningful way, clinicians are spending less time navigating through DocToDoor and more time understanding patient condition. By enabling clinicians to create patient care routines with easy to use interface, clinicians can automate many functions & aspects of care management. Upon reduction in the effort, clinicians will be provided patient-feedback with information rich platform that will aid in decision-making and situational awareness. Considering that patients spend most of their time outside a healthcare facility, it is critical that clinicians be aware of what and how the patient is feeling.
By gaining consistent feedback from clinicians and patients, we improve usability of DocToDoor to improve user experience. By understanding what clinicians are really trying to achieve and what patients really want, we can design features that meet the needs and expectations of the end-users as opposed to what we, as digital health innovators, think they want.
Reducing the efforts our users must undertake, improving the information they see, and automating functions otherwise performed by people enable us to ensure that DocToDoor is platform for managing and administering better care. A telehealth platform such as DocToDoor is a tool to help make healthcare better, not solve healthcare; as digital health developers, the best we can do is listen to clinicians and patients.
Final Remarks
The surge at which digital health/telehealth industry is developing new systems is difficult for Clinicians, Patients, and Healthcare Organizations to keep. Organization may inundate Clinicians with myriad of systems to fulfill clinical and operational needs leaving Clinicians frustrated and burdened. Considering that both the digital health industry and healthcare organizations often consider user needs as an afterthought, a renewed approach is needed where user needs and human-centered design are on the forefront of digital health transformation. Healthcare has spent decades coping with inefficient systems, isn’t it about time we change that.
Share:
About DocToDoor
DocToDoor is a custom branded Telehealth solution designed to empower physicians to manage care through the entire care continuum for post-visit, chronic care, and post-op recovery. We are empowering physicians with user-centric remote patient monitoring & engagement and telemedicine platform to manage and care for patients through the entire breadth of patient-provider relationship.