Remote Patient Monitoring Systems: A Practical Guide for Healthcare Providers (2026)
Learn how remote patient monitoring systems help healthcare providers track patient health in real time, improve outcomes, reduce readmissions, and deliver better care in 2026.
Healthcare is no longer limited to clinics and hospitals. Care now continues even after patients go home, and that is where remote patient monitoring systems make a real difference.

For healthcare providers, the challenge is not just treating patients but staying connected with them between visits. Remote patient monitoring helps close that gap. It allows clinicians to track health in real time, step in earlier when needed, and provide more consistent care without adding extra workload.
As healthcare moves toward better outcomes and long-term care, remote monitoring is no longer just a trend. It is becoming an essential part of everyday practice.
An Overview of Remote Patient Monitoring Systems
Remote patient monitoring systems are digital healthcare solutions that enable providers to monitor patients' health outside clinical settings through connected devices and software.
These systems collect data such as blood pressure, glucose levels, oxygen saturation, and weight, then send it securely to a centralized platform. Providers can review this data, identify risks, and take action without requiring in-person visits.
In simple terms, it allows you to stay clinically connected to your patients even when they are at home.
Why it matters now
- Patients expect more convenient care
- Chronic conditions require continuous monitoring
- Providers need better visibility between visits
- Healthcare systems are under pressure to reduce readmissions
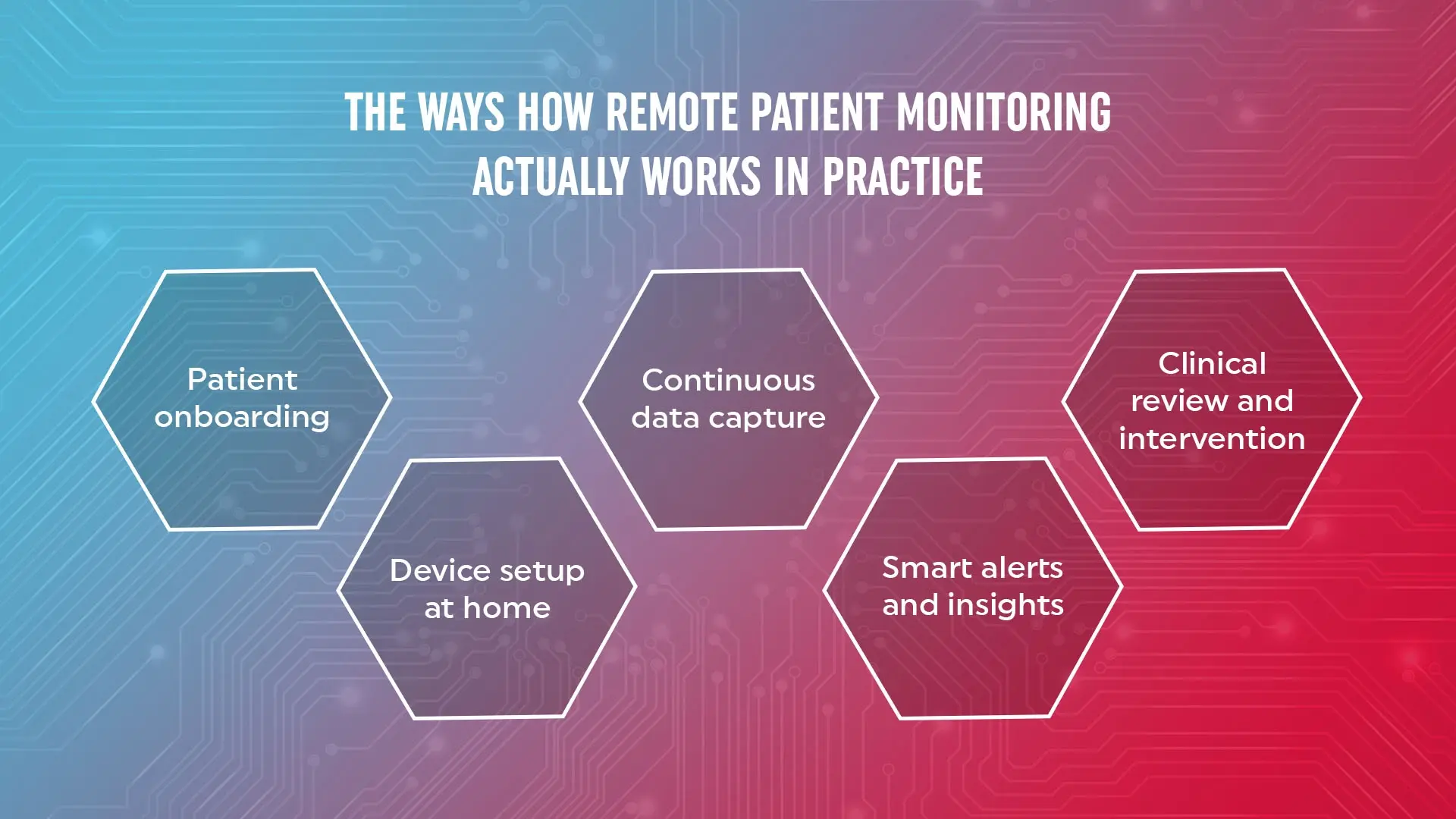
How Remote Patient Monitoring Actually Works in Practice
Understanding the workflow helps clarify why RPM is so effective.
1. Patient onboarding
Patients are enrolled based on their condition, such as diabetes, hypertension, or post-discharge recovery. A care plan is defined from the start.
2. Device setup at home
Patients receive easy-to-use devices. These are typically pre-configured so patients can start using them without technical difficulty.
3. Continuous data capture
Devices automatically record health data and send it to the platform. This removes the need for manual tracking.
4. Smart alerts and insights
The system analyzes incoming data and flags anything outside normal ranges. This helps providers focus only on patients who need attention.
5. Clinical review and intervention
Care teams monitor dashboards and respond when needed. This could be a quick call, medication adjustment, or escalation.
What Makes a Remote Patient Monitoring System Reliable?
Not all RPM solutions deliver the same value. The most effective systems combine simplicity, automation, and clinical intelligence.
Connected medical devices
Reliable devices are the foundation. These include blood pressure monitors, glucose meters, pulse oximeters, and smart scales that automatically transmit data.
Intelligent monitoring platform
The software should not just collect data but make it useful. Look for real-time alerts, trend analysis, and easy-to-read dashboards.
Patient-friendly experience
If patients find the system difficult to use, adoption drops. Simple apps, reminders, and clear instructions make a big difference.
Clinical dashboards that prioritize care
Instead of overwhelming providers with data, good systems highlight high-risk patients first. This improves efficiency and response time.
Real Benefits for Healthcare Providers
Remote patient monitoring is not just about technology. It directly impacts how care is delivered.
Better patient outcomes
Continuous monitoring allows earlier intervention. Small issues can be addressed before they become serious complications.
Fewer hospital readmissions
Post-discharge monitoring helps ensure patients recover safely, reducing the risk of readmission.
Stronger patient engagement
When patients track their own health, they become more involved in their care. This improves adherence to treatment plans.
More efficient care delivery
Providers can monitor multiple patients without increasing in-person visits. This helps optimize time and resources.
Financial sustainability
RPM programs align with reimbursement models supported by organizations like the Centers for Medicare & Medicaid Services, making them a viable long-term investment.
Areas Where Remote Patient Monitoring Systems Play a Crucial Role
Chronic disease management
Conditions like diabetes and hypertension require consistent monitoring. RPM provides ongoing visibility without frequent clinic visits.
Cardiac care
Patients with heart conditions can be monitored for irregularities, helping prevent emergencies.
Post-hospital recovery
Patients recovering from surgery or illness can be tracked closely, reducing complications and readmissions.
Elderly and home care
RPM supports independent living while ensuring safety through continuous monitoring.
Choosing the Right Remote Patient Monitoring System
Selecting the right platform is critical for better decision-making and faster recovery. Here are a few factors you can consider:
Keep it simple
Choose a system that is easy for both patients and providers. Complexity reduces usage.
Ensure device compatibility
The platform should integrate seamlessly with multiple medical devices to ensure accurate data collection.
Prioritize data security
Patient data must be protected under standards like the Health Insurance Portability and Accountability Act (HIPAA).
Why More Providers Are Moving Toward RPM
Healthcare providers are under constant pressure to do more with less. Remote patient monitoring helps address this challenge. It reduces unnecessary hospital visits, improves continuity of care, and allows providers to focus on patients who need attention most.
At the same time, patients are becoming more comfortable with digital care. They prefer solutions that fit into their daily lives rather than requiring frequent clinic visits.
This combination of provider need and patient expectation is driving rapid adoption of RPM.
How DocToDoor Supports Smarter Remote Care
Remote patient monitoring systems are not just an upgrade to existing care models. They represent a shift in how care is delivered. For healthcare providers, the real value lies in staying connected with patients beyond the clinic, making faster decisions, and improving outcomes without adding complexity.
At DocToDoor, we focus on making this shift simple and practical. Our app and devices are built to help you monitor patients in real time, identify risks early, and take timely action without adding extra workload to your team.
We combine easy-to-use devices, smart alerts, and clear dashboards so you can focus on what matters most and deliver better care. From supporting post-discharge monitoring to managing chronic conditions, our goal is to help you stay connected with your patients at every step.
As healthcare continues to evolve, adopting the right RPM system can help you deliver more proactive, efficient, and patient-centered care, and with solutions like ours, it becomes much easier to put that into practice.
Frequently Asked Questions
Do patients find RPM difficult to use?
Most modern systems are designed to be simple, with minimal setup and easy-to-use devices.
What conditions benefit most from RPM?
Chronic conditions like diabetes, hypertension, and heart disease benefit the most.
Is RPM reimbursable?
Yes, many RPM services are reimbursable under programs defined by the Centers for Medicare & Medicaid Services.
What should I look for in an RPM platform?
Ease of use, strong device integration, data security, and actionable insights are key factors.