
Redesigning How We Provide Healthcare – Some takeaways from IHI Summit
As a domain, healthcare is essentially a very much human-centered field, whether it is the patient or the clinician – both groups have different needs and requirements. Yet, for the longest time, healthcare has been delivered void of human-centered approach. Patients needs and desires are unmet or not considered; provider needs are overlooked for administrative and organizational needs. In the midst of this, what is left is a system that remains burdened and far removed from user needs.
Population Health and Human-Centered Design
Reimagining and redesigning healthcare should be a simple and uncluttered process involving all major stakeholders and users. Recently, at the Institute of Healthcare Improvement (IHI) 18th Annual Summit on Improving Patient Care in the Office Practice and the Community, we had a close up view of how healthcare systems across the nation are revamping care delivery to better care for their population. The prime focus was on using human-centered design as an innovative approach to design care that meets the needs of the population and meet their patients where they are. Workshops and presentations focused on learning the needs of your population and tackling the problem upstream.
Children’s Health System out of Texas used human-centered design to build a care delivery model that took family and community needs into account, discovered ‘upstream’ challenges for families that affected children’s health, and provided solutions & engagement strategies to reduce long-term risks for children. For Children’s Health, the focus was on reducing chronic health problems amongst children by:
(a) enabling access to affordable nutritious food,
(b) educating parents about how to prepare healthy food options,
(c) understanding barriers faced by families for a healthier lifestyle, and
(d) working with community partners to remove barriers. By addressing the problem ‘upstream’, eventual risks to child population can be reduced.
In the above example, human-centered design was used to support an entire population. But what about the individual patients?
Human-Centered Design for Individual Care
Designing care around individual patients needs to incorporate the following:
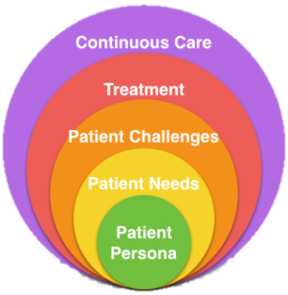
- Who is your patient? Build their persona, have some fundamental concepts of their lifestyle
- What does this patient need? What does the patient need and want versus what you think they need? There could be significant differences in what the patient wants versus what they actually need. The crux here is to understand what are their concerns related to their health and what they would like to achieve from each visit.
- What are the challenges faced by your patient? It could be lack of transportation or financial constraints related to nutrition and medication. What about their emotional and behavioral health? Do they have a support system? A family? Challenges faced by patients can undermine and greatly impact their health.
- Developing a treatment by taking the above into consideration, the patients are likely to be more satisfied with their visits and more engaged in their health.
- Communicate and collaborate continuously between every visit. Telehealth and mHealth platforms can provide tremendous support to maintain effective care and remain connected to your patient.
The IHI Summit provided valuable insight and lessons for developing innovative models of care. If healthcare is to succeed in collaborating with and improving patient health, we must rethink how we deliver care and view patients.
About DocToDoor
DocToDoor is a custom branded Telehealth solution designed to empower physicians to manage care through the entire care continuum for post-visit, chronic care, and post-op recovery. We are empowering physicians with user-centric remote patient monitoring & engagement and telemedicine platform to manage and care for patients through the entire breadth of patient-provider relationship.


